Preventing Respiratory Issues in Seniors: From Allergies to COPD
Why Every Breath Matters & Get Expert Tips – Manage COPD and Respiratory Health
As we age, taking care of our lungs becomes more critical. Seniors are more likely to face breathing problems like allergies, asthma, and chronic obstructive pulmonary disease (COPD), which can make daily life difficult. Simple things, like dust and indoor air pollution, can trigger asthma attacks, especially since older adults tend to spend more time indoors. Managing COPD also requires proper inhaler use, but studies show that less than 20% of seniors use inhalers correctly, meaning many don’t get the full benefit of their medication. On top of that, respiratory infections can quickly worsen existing lung problems and lead to serious health risks. Therefore, maintaining healthy lungs for seniors requires a multifaceted strategy that includes avoiding allergens, taking medications as prescribed, and avoiding infections.
Understanding Manage COPD
Chronic Obstructive Pulmonary Disease (COPD) is a progressive lung condition that makes breathing increasingly difficult. Its two main conditions are chronic bronchitis and emphysema, both of which obstruct airways and limit airflow. While COPD is most associated with smoking, long-term exposure to air pollution, dust, and chemicals can also contribute to its development.
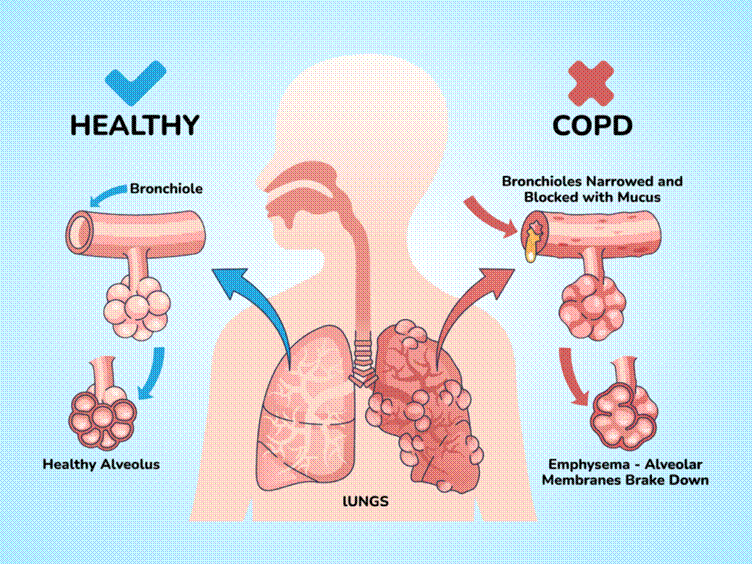
Symptoms of COPD
The symptoms of COPD often develop gradually and worsen over time. Common signs include:
- Persistent cough that produces mucus (chronic bronchitis)
- Wheezing due to airway narrowing
- Fatigue caused by reduced oxygen supply
- Shortness of breath, especially during physical activities
- Difficulty recovering from colds or respiratory infections
- Feeling winded after simple tasks like climbing stairs
Why Seniors Are More at Risk for Breathing Problems

- Weaker Lungs with Age: As we grow older, our lungs lose strength and elasticity, making deep breathing more difficult. The muscles that support breathing also weaken, leading to shortness of breath, even with mild activity.
- Narrower Airways and Increased Mucus: Aging causes airways to become slightly narrower and produce more mucus, which can trap allergens, dust, and bacteria. This increases the risk of allergies, infections, and chronic breathing difficulties.
- Weakened Immune System: The body’s ability to fight infections declines with age, making seniors more vulnerable to respiratory illnesses like pneumonia and the flu. These infections can quickly become severe if not managed properly.
- Environmental and Lifestyle Factors: Long-term exposure to pollution, smoking (even second-hand smoke), and indoor allergens can worsen conditions like asthma and COPD. Since many seniors spend more time indoors, poor air quality can have a significant impact on their lung health.
Recognizing these risks is the first step in preventing serious respiratory issues. By making simple adjustments to daily habits, seniors can protect their lungs and breathe more easily.
Tips to Prevent Respiratory Issues
Avoid Environmental Triggers
Seniors should minimize exposure to allergens and pollutants that can trigger asthma and other respiratory issues. Reducing indoor allergens, including dust mites, pet dander, and mold, while avoiding outdoor pollutants like pollen and vehicle emissions, is essential. Regular cleaning and the use of air purifiers can help maintain improved indoor air quality.
Proper Inhaler Use
For seniors with COPD or asthma, using inhalers correctly is crucial for effective treatment. Many elderly patients struggle with proper inhaler techniques, reducing the medication’s effectiveness. Regular training and technique reviews with healthcare professionals can lead to better disease management.
Vaccinations
Staying up to date with flu and pneumonia vaccinations is vital in preventing respiratory infections, which can worsen conditions like asthma and COPD. Seniors are more vulnerable to infections due to age-related immune system changes, making vaccinations an important preventive measure.
Respiratory Rehabilitation
Participating in respiratory rehabilitation exercises can improve lung function and reduce symptoms in seniors with COPD. These exercises enhance breathing efficiency, alleviate breathlessness, and improve overall endurance.
Healthy Lifestyle Choices
A well-balanced diet and regular physical activity contribute to stronger lung function. Avoiding smoking is particularly crucial because smoking is a significant risk factor for COPD and other respiratory conditions.
Monitor Air Quality
Seniors should stay informed about air quality levels, particularly on high pollution days. Staying indoors when air quality is poor and using air conditioning can help minimize exposure to harmful particles that may worsen respiratory conditions.
Regular Medical Check-ups
Routine check-ups with healthcare providers help in the early detection and management of respiratory issues. This is especially important for seniors with a history of lung-related problems, as timely intervention can prevent complications.
Seniors can improve their overall quality of life and lower their risk of flare-ups by using these strategies to better manage their respiratory health.
Role of Nutrition in Respiratory Health – COPD
A healthy diet is essential for preserving lung function and averting respiratory problems. Nutrient-rich foods help reduce inflammation, support immune function, and enhance overall lung capacity. Seniors should focus on consuming antioxidant-rich fruits and vegetables like berries, spinach, and carrots, which help protect lung tissues from damage. Walnuts and flaxseeds contain omega-3 fatty acids, which can help lower airway inflammation and facilitate breathing.
Maintaining adequate hydration is equally important because it thins mucus, making it easier to clear the airways. Seniors should also limit their intake of processed foods and excessive salt because these foods can worsen breathing issues and fluid retention. By choosing their food carefully, seniors can improve their respiratory systems and reduce their risk of lung health issues.
Pulmonary Rehabilitation: A Game Changer for COPD Management
Pulmonary rehabilitation is one of the most effective ways for people with COPD to improve their breathing, build stamina, and enhance overall well-being. This structured program combines exercise training, education, and breathing techniques to help individuals manage their symptoms and stay active.
How Pulmonary Rehabilitation Helps
- Improves lung efficiency: Guided exercises strengthen respiratory muscles, making breathing easier over time.
- Reduces breathlessness: Training in controlled breathing techniques like pursed-lip breathing helps manage shortness of breath.
- Boosts endurance: Gradual increases in physical activity enhance overall stamina, reducing fatigue.
- Provides emotional support: COPD can be mentally challenging, but rehabilitation programs often include counselling and support groups to help individuals cope.
- Teaches effective symptom management: Participants learn ways to recognize warning signs of exacerbations and act before symptoms worsen.
Who Should Consider Pulmonary Rehab?
Anyone with moderate to severe COPD or chronic lung disease who experiences frequent breathlessness can benefit. Pulmonary rehab is often recommended for individuals who struggle with daily activities like climbing stairs, walking long distances, or carrying groceries.
By incorporating pulmonary rehabilitation into COPD management, individuals can regain confidence in their breathing, stay active, and improve their overall quality of life.
How mySeniorCareHub Can Help Manage COPD and Respiratory Health
Managing COPD and chronic lung issues requires continuous monitoring, timely intervention, and lifestyle adjustments. mySeniorCareHub offers a comprehensive healthcare solution designed to support seniors in maintaining their respiratory health.
- Personalized Health Monitoring: The Wellness Score feature tracks vital signs like oxygen levels, pulse rate, respiration rate, and overall lung health, helping seniors and caregivers detect early signs of respiratory distress.
- Medication Reminders: Many seniors struggle with medication adherence, which is critical for COPD management. mySeniorCareHub smart reminders ensure timely use of inhalers, oxygen therapy, and prescribed medications.
- Emergency Alerts & GPS Tracking: Sudden breathlessness or flare-ups can be life-threatening. The app provides real-time emergency alerts with GPS location sharing, allowing immediate assistance from caregivers or emergency services.
Seniors with COPD can improve their overall quality of life, decrease hospitalizations, and better manage their illness by incorporating mySeniorCareHub into their daily routine.