What If Your Parent Faces a Medical Emergency Alone?
Imagine this: your mother, living alone, collapses from a stroke. She can’t reach her phone, and no one is around. The clock starts ticking. In cases like this, every minute without medical alert increases the risk of permanent brain damage or death. It’s a chilling scenario, but sadly not uncommon among elderly individuals. As families juggle work, caregiving, and long-distance living, this question becomes frighteningly real. This article examines how emergency alerts and real-time location tracking via mySeniorCareHub and similar platforms can help close the gap between immediate care and isolation.
Everyone Should have this Best Emergency & Medical Alert App.
Why Every Minute Matters in Medical Emergencies
Stroke, cardiac arrest, and diabetic complications are leading causes of morbidity in the elderly. What makes them life-threatening is how fast they escalate.
| Medical Event | Critical Time Window | Outcome of Delayed Help |
| Stroke | Within 60 minutes (Golden Hour) | Increased risk of paralysis, cognitive decline |
| Cardiac Arrest | Within 4-6 minutes | Permanent brain damage, death |
| Diabetic Hypoglycaemia | Within 15-30 minutes | Seizures, unconsciousness, coma |
These emergencies don’t wait. Yet most elderly individuals, especially those living alone, are unprepared to signal for help quickly.
Barriers Faced by Families and Seniors
Even attentive families face limitations:
- Elderly loved ones may be reluctant to call for help.
- Phones may not be reachable during an emergency.
- Caregivers can’t always be present.
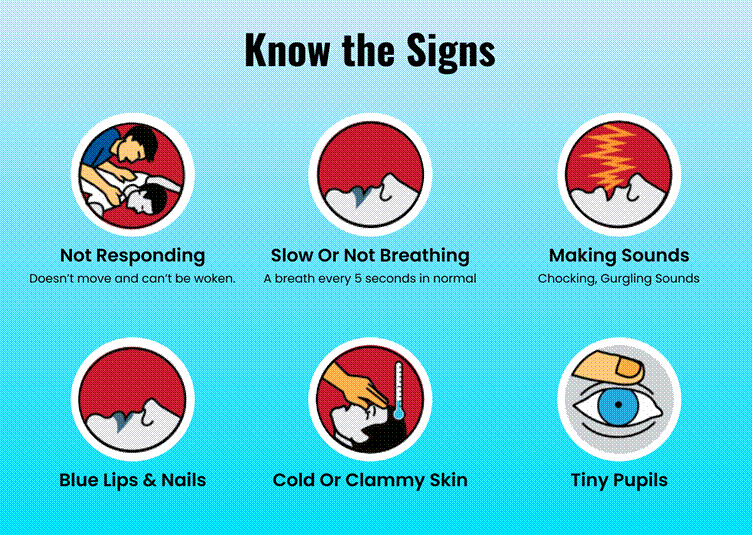
- Many seniors downplay early symptoms, losing precious time.
These challenges call for an intelligent system that doesn’t rely solely on the patient raising an alarm.
How Medical & Emergency App Works
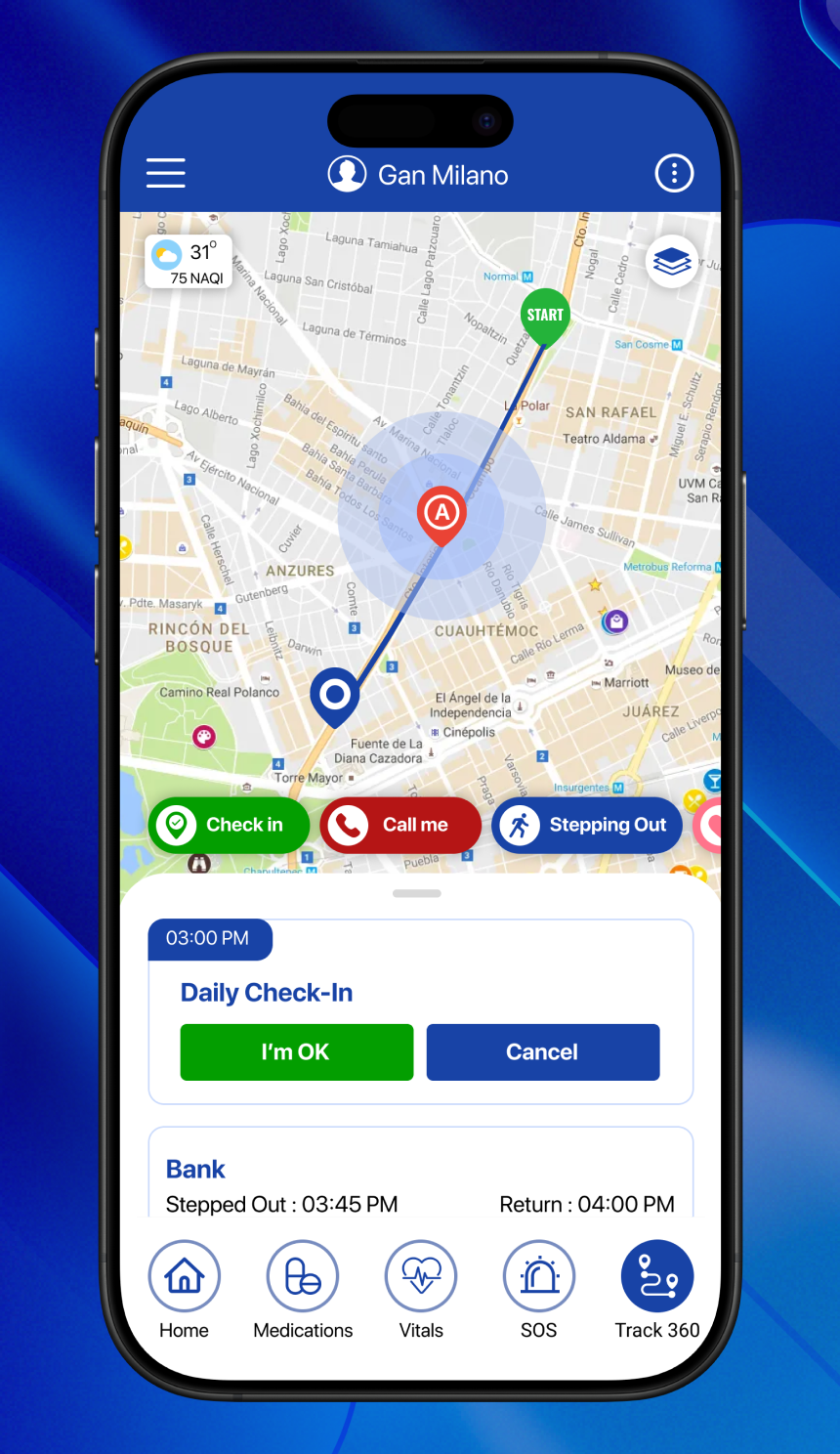
With modern digital health tools, we no longer rely entirely on verbal communication during a crisis. Here’s how location-enabled platforms like mySeniorCareHub provide an active safety net:
| Feature | Function |
| GPS Location Tracking | Continuously monitors seniors’ real-time location |
| Fall Detection | Auto-detects sudden movement or impact |
| Emergency Alerts | Instantly notifies family and emergency services |
| Geo-Fencing | Alerts when a senior moves out of a safe zone |
| Health Monitoring Integration | Tracks vitals like heart rate, glucose, BP, etc. |
This multi-layered support system ensures that help is on the way even when the elder cannot speak or move.
mySeniorCareHub: Best Emergency & Medical Alert App
mySeniorCareHub combines technology and compassion. It has been specifically designed for geriatric health needs. Here’s how it stands apart:
- Live Location Monitoring: Tracks elders in real-time, helping locate them instantly during emergencies.
- Emergency Contact Integration: Automatically shares live coordinates with designated family members and ambulance services.
- Instant Alerts: Sends push notifications, calls, and SMS when an abnormal event is detected.
- Vital Signs & Wellness Score: Monitors vital parameters and assigns a score to help assess health trends over time.
“Our goal was to create a platform that acts when you can’t. mySeniorCareHub is not just an app. It’s a lifeline.”
Stroke Detection in Action –Best Emergency & Medical Alert App
Consider this example:
Mrs. Meena, 74, lives in Chandigarh. One afternoon, she experiences slurred speech and collapses. Her mySeniorCareHub device detects a fall and triggers an emergency alert. Her son receives a push notification with a live GPS link. Within 3 minutes, the system contacts the local ambulance service with her coordinates. Medical help arrives in under 12 minutes. Doctors later confirmed she was treated well within the golden hour.
It’s the power of proactive care.
Medical Perspective: Why It Works
- Neurological Events (e.g., Stroke): Early thrombolytic therapy within 3 hours drastically improves outcomes. Real-time alerts accelerate this timeline.
- Diabetic Emergencies: Immediate response can prevent coma and hospitalisation.
- Cardiac Arrest: CPR or defibrillation within the first 6 minutes significantly increases survival rates.
With location tracking, these interventions are no longer delayed due to logistical confusion or unreachable phones.
Emotional and Practical Reassurance for Families
The emotional toll of caregiving can be heavy. Constant worry, guilt, and fear of missing an emergency moment can drain families. Real-time tracking provides:
- Peace of Mind: You’re always informed, no matter where you are.
- Autonomy for Elders: Seniors retain independence while staying safe.
- Faster Emergency Response: Coordinated care teams can act without waiting for human-initiated calls.
Conclusion
A stroke, a fall, or a diabetic episode doesn’t have to end in tragedy. Technology today gives us tools that didn’t exist a decade ago. With mySeniorCareHub’s real-time tracking and emergency alert system, you’re never truly far from your loved one’s side. It transforms helplessness into readiness.
In moments where every second counts, knowing where your parent is—and that help is already on the way—is more than peace of mind. It’s lifesaving.
Explore the emergency features and real-time monitoring tools of mySeniorCareHub. Because when your loved one is in danger, you deserve to know—and act—in real time.